Couple Years of Protection:
1,59,72,012: Male Condom
14,53,802: OCP
18,75,063: IUCD
7,839: Male Sterilisation
13,26,949: Female Sterilization
27,325: Injectable – DMPA
Dr Hema Divakar is an accomplished Obstetrician & Gynaecologist with 26 years of experience. She has held the prestigious office of the President of the Federation of Obstetrics and Gynecological Societies of India (FOGSI). Currently, she practices at Divakar’s Speciality Hospital, Bangalore
ÔÇ£While provision of services is important for improving Reproductive & Child Healthcare, it is equally important to invest in quality enhancement of those services. Raising the quality of care has a significant impact on reducing maternal, neonatal and infant mortalitiesÔÇØ
Family Planning, Safe Abortions, Antenatal & Postnatal Care and Institutional Deliveries by Skilled Health Attendants are proven steps to prevent Maternal Deaths. Similarly, Neonatal Resuscitation, Early Initiation of Breastfeeding & Immunisation, Timey Treatment of Infections among newborns, Extra Monitoring of Low Birth Babies, etc, can go a long way in avoiding deaths among newborns and infants.
However, merely increasing access or provision of these services is not sufficient unless due emphasis is also placed on quality enhancement of such services. In fact, multiple global deliberations at policy and implementation levels have drawn a unanimous consensus that increasing quality of Reproductive & Child Healthcare (RCH) has a considerable bearing on reducing maternal, neonatal and infant mortalities.
Improving quality of care improves service delivery, client satisfaction and trust, thus leading to increased footfalls at health facilities and better health outcomes. However, ÔÇÿqualityÔÇÖ is a subjective matter and its connotation varies with stakeholders. Patients & their attendants, communities, healthcare providers, administrators and government ÔÇô all perceive ÔÇÿquality of careÔÇÖ differently. For instance, satisfaction level of Patients rests on ÔÇÿservicesÔÇÖ ÔÇô immediate relief or cure from diseases, speedy recovery, clean atmosphere, courteous behaviour of staff, etc. Usually they do not judge quality on technical parameters. But Health Service Providers often equate quality with technical performance. Similarly, Community or Society defines quality as protection of health rights of the underprivileged, whereas administrators perceive quality as compliance with clinical guidelines/protocols and optimum utilisation of resources.
To bring standardisation in quality of care, several international bodies have devised standards, guidelines and protocols. The Ministry of Health and Family Welfare, Government of India, has placed ÔÇÿOperational Guidelines for Quality Assurance in Public Health FacilitiesÔÇÖ. As per the Guidelines, Quality of Care can broadly be classified into Technical and Service Components. Technical Quality is mostly the concern of Health Service Providers (doctors, nurses, paramedical staff, etc). It includes Clinical Protocols, Infection Control, Emergency Response, etc, that impact Service Delivery or Outcome of Services. On the other hand, Service Quality includes Prompt Service Delivery, Courteous Behaviour of Staff, Hygiene & Cleanliness, Privacy and Dignity, etc. These largely determine patientsÔÇÖ experience and have a bearing on Client Satisfaction Levels.
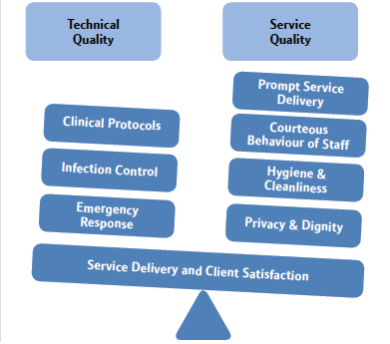
Source: Operational Guidelines on Quality Assurance in Public Health Facilities, 2013, Ministry of Health and Family Welfare, Government of India
The Guidelines have further defined Eight ÔÇÿAreas of ConcernÔÇÖ that Measure Quality of a Health Facility, namely: Service Provision, Patient Rights, Inputs, Support Services, Clinical Care, Infection Control, Quality Management and Outcome. These are further categorised into 70 Standards, each having Specific Measurable Elements and Department-Specific Checkpoints.
Among these, Clinical Care is particularly significant for RCH services. Hence, out of 23 Standards listed under Clinical Care, a set of seven Standards is especially dedicated to clinical processes for Maternal, Newborn, Child, Adolescent and Family Planning services and National Health Programmes.
RCH Standards under Clinical Car
that ensure ÔÇÿThe Facility has Established ProceduresÔÇÖ for
Antenatal Care: ANC Registration, Identification of High-Risk Pregnancy, Management of Anaemia, Pregnancy Care Counselling, Processes during Check-ups, etc
Intra-natal Care: Clinical Processes for Normal Delivery, Management of complications and C-Section Surgeries, Active Management of 3rd Stage of Labour, Neonatal Resuscitation, etc
Postnatal Care: Postnatal Maternal Care and Neonatal, Prevention of Hypothermia, Breastfeeding Initiation, etc
Care of Newborn, Infant and Child: Immunisation, Management of Newborn & Childhood Illnesses such as Jaundice, Asphyxia, Low Birth Weight, Sepsis, Diarrhoea, Malnutrition, etc
Abortion & Family Planning: As per Govt Guidelines and Law, Family Planning Counselling, Spacing Methods, FP Surgeries, Counselling & Procedures for Abortions, etc
These apart, Standards are also laid to ensure the Facility Provides: Adolescent, Reproductive & Sexual Health Services, and National Health Programmes
*Source: Assessor’s Guidebook for Quality Assurance in District Hospitals 2013, Minsitry of Health and Family Welfare, Govt of India
These are measures that can go a long way in protecting the lives of millions of young mothers, newborns and infants. However, compliance of these Standards and Guidelines is not just a State Mandate. In fact, this is the collective responsibility of all stakeholders of the healthcare sector including Public and Private Health Facilities, NGOs, Research Institutes, Policy Makers, Administrators, International Donor Agencies, as well as the Corporate Sector to assist the Government is fulfilling this incredible goal.
HLFPPT has instituted Merrygold Health Network (MGHN) which is largely focused on RCH. With 700+ health facilities, 800+ doctors and 12,000+ community health volunteers across seven states, MGHN is IndiaÔÇÖs largest social franchising health network based on Public Private Partnership. Over the years, the network has successfully provided 2 million ANCs, 0.6 million institutional deliveries and family planning counselling to nearly 1.5 million clients. As the network has plans for further expansion on self-sustainable model, quality of care shall be a significant determinant of growth. Helping such a health network with quality enhancement tools and providing guidance that can improve competencies and capabilities of its Healthcare Providers and health facilities becomes paramount for research institutes. Let us all work together to Raise the Bar!
The column originally appeared in Samvad Magazine (Apr-June 2016 issue)